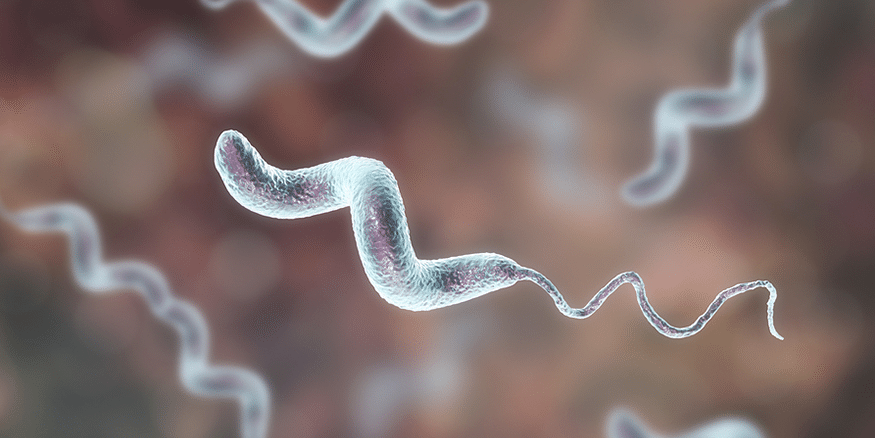
Campylobacter
Campylobacter is a species of bacteria that is one of the leading causes of foodborne diarrheal disease in the modern world. Although their Salmonella and E. coli cousins have become engrained in the minds of wary hamburger-eaters everywhere, this lesser known genus of bacteria has not garnered as much attention. This is surprising given reports suggesting that Campylobacter is responsible for approximately 5% of patients with diarrhea, a statistic that exceeds that of Salmonella infections.1
What are Campylobacter and where do they come from?
Campylobacter coli and Campylobacter jejuni are the two major subtypes of Campylobacter responsible for foodborne caused diarrhea. They are thin, spiral shaped, gram-negative rods that are capable of moving with a characteristic corkscrew motion. Campylobacter infection in humans is generally attributed to contaminated livestock and poultry that is undercooked when consumed.2 Although free of infection at birth, farm animals have significant counts of Campylobacter in their intestines by the time they reach slaughter via infection from the environment and other animals. Contact with fecal matter at the time the animal is killed can contaminate meat products with infective doses of Campylobacter. In recent years, the food industry has made significant efforts to promote proper food handling ‘from farm to fork’. While refrigeration of meat and dairy products inhibits the growth of Salmonella and E.coli cultures, interestingly, recent studies have suggested that these also happen to be the best conditions to keep Campylobacter cultures viable for infection.3
How does Campylobacter cause diarrhea?
There have been several proposed models of Campylobacter infection but all generally involve bacterial attachment to the mucosal lining of the gut via specialized proteins, followed by invasion and toxin production. Of the several toxins produced by Campylobacter, only the cytolethal distending toxin (Cdt) has been studied at the molecular level and has been indicated as having an integral role in pathogenesis.4 It is believed that Cdt initiates DNA degradation, which causes cells to arrest in what is known as the G2 stage of the cell cycle and subsequently die.5 It has been hypothesized that this particularly occurs in the crypt structures of the intestine where cells are normally rapidly dividing. The death of these specialized cells is thought to lead to the loss of function and erosion of the protective intestinal epithelial layer thus producing the electrolyte disturbances and malabsorption associated with diarrhea. Recent research has also acknowledged that Campylobacter strains have developed a variety of unique functions that assist in their ability to infect a host, including: unique surface proteins that aid in adhesion and evasion from the host’s immune system; defences to oxidative stresses used by immune cells to kill the bacteria; and, a phenomenon known as quorum sensing whereby chemical factors are used as communication signals with other bacterial species to coordinate infection.6
What are some long-term effects of Campylobacter infection?
Campylobacter infection has been associated with a number of autoimmune diseases including arthritis (particularly affecting the knee joint), Reiter’s syndrome (a form of arthritis affecting the spine), conjunctivitis, and Guillain-Barré syndrome (a paralysing inflammatory disorder of the peripheral nerves). However, these chronic sequelae are rare and have a frequency of less than 1% following infection.7















